|
Health problems do not usually occur during an Rh-negative person’s first pregnancy with an Rh-positive fetus, as the body is unlikely to produce enough anti-D antibodies. Some people may refer to this as Rh disease. These antibodies can cross the placenta and attack the fetus’s blood cells. When a person who is Rh-negative is pregnant with an Rh-positive fetus, their body will recognize the Rh-positive blood as foreign and produce anti-D antibodies. This may occur during pregnancy or if a person accidentally receives incompatible blood during a transfusion. The main complication relating to Rh factors involves those who are Rh-negative encountering Rh-positive blood and producing anti-D antibodies in response. However, it can influence their compatibility with other blood types, affecting the type of blood they can receive. While being Rh-positive is more common, being Rh-negative does not indicate illness, and it does not usually affect a person’s health. The positive or negative sign next to the ABO grouping refers to the Rh status and whether the RhD antigen is present or not. Combining these systems creates the eight most common blood types: People with no A or B antigens on the surface of their RBCs have blood type O. 
The absence or presence of A or B antigens and Rh factor can help classify blood types. RBCs contain proteins, or antigens, on their surface that allow specialists to determine blood types. Although Rh status can vary among populations, roughly 85% of people in the United States are Rh-positive. People inherit their Rh status from their parents, separate from their ABO blood type. The Rh D antigen is the most immunogenic, meaning that it may provoke an immune response. There are five main Rh antigens on RBCs, of which the most important is the Rh D antigen. The Rh factor is an inherited protein that can be present on the surface of RBCs. In RBCs, RhAG may transport NH(3) to detoxifying organs like kidney and liver and with non-erythroid tissues orthologs may contribute to regulation of the acid-base balance.Share on Pinterest Yothin Sanchai/EyeEm/Getty Images The crystallographic structure of the bacterial ammonia channel AmtB and functional studies showing that AmtB conducts NH(3) into reconstituted vesicles is fully consistent with these latter studies. Furthermore, recent studies performed in human and murine red blood cells (RBC) indicate that RhAG facilitates CH(3)NH(2)/NH(3) movement across the membrane and represents a potential example of gas channel. 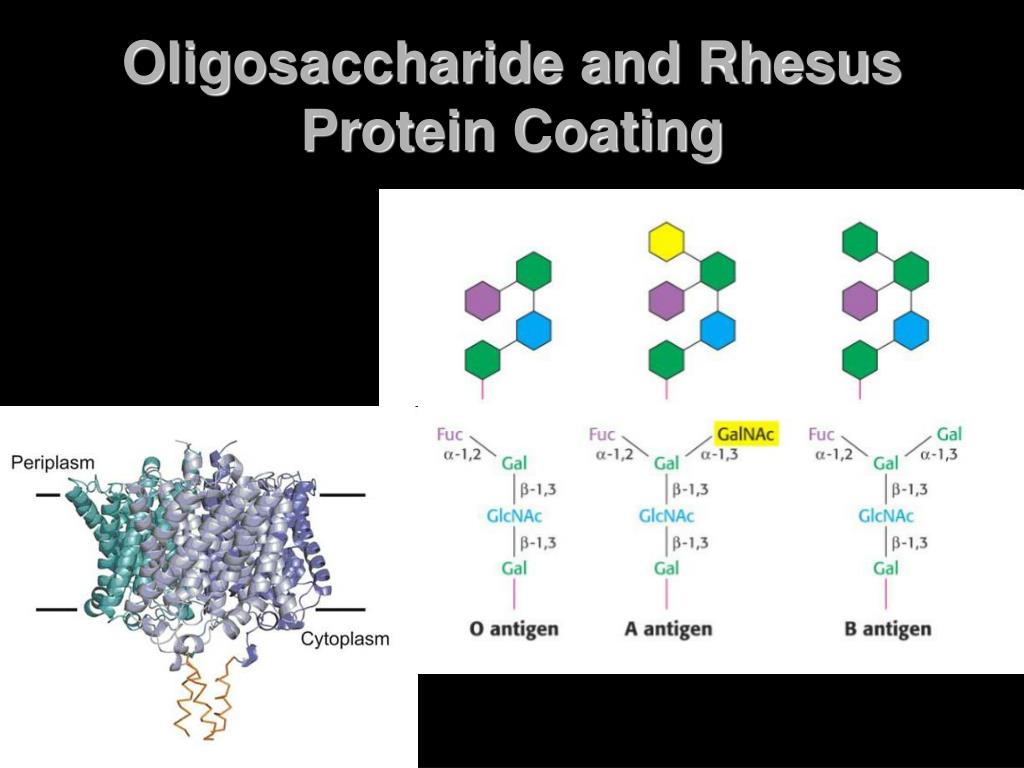
Functional analyses in heterologous systems revealed that RhAG, RhBG and RhCG can mediate ammonium (NH(3) and/or NH(4)(+)) transport across the cell membrane and might represent mammalian specific ammonium transporters. 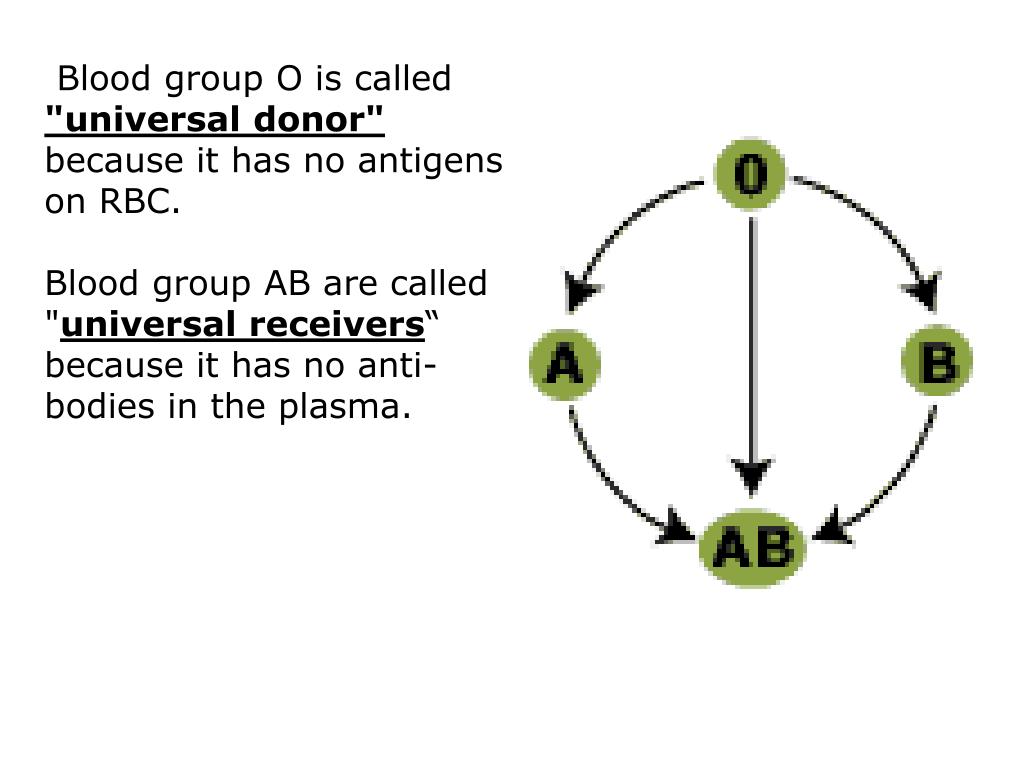
In mammals, the Rh protein family includes two non-erythroid members, RhBG and RhCG, mainly expressed in liver and kidney, two organs specialized in ammonia genesis and excretion. The demonstration that the RHD-positive locus is composed of the RHD and RHCE genes, whereas the RHD gene is deleted in most RhD-negative individuals, allowed fetal RhD genotyping by non-invasive PCR assays for antenatal diagnosis of pregnancy at risk for Rh hemolytic disease of the newborn. Molecular basis of most Rh phenotypes, including the Rh(null) phenotype associated with hemolytic anemia, have been determined. The RH system is one of the most immunogenic and polymorphic human blood group system. By interacting with the spectrin-based skeleton through protein 4.2 and ankyrin, the Rh complex contributes to the maintenance of the mechanical properties of the erythrocyte membrane. Rh (Rhesus) proteins (D, CcEe) are expressed in red cells (RBC) in association with other membrane proteins (RhAG, LW, CD47 and GPB).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
